COVID 19 Task Force Update – Medical Exemptions
The COVID -19 Primary Care Taskforce have released their latest update expressing concerns about reports of bulk vaccine exemptions being issued by some Doctors and warming against this.
The COVID -19 Primary Care Taskforce have released their latest update expressing concerns about reports of bulk vaccine exemptions being issued by some Doctors and warming against this.
Terms of Reference
That this House requires the Legal and Social Issues Committee to inquire into, consider and monitor the capacity and fitness for purpose of the Victorian Government’s COVID‐19 contact tracing system and testing regime, and in doing so consult with businesses, including small business representatives, the community sector and Victoria’s multicultural communities, and provide a report to the House no later than 14 December 2020.
Presenter: Dr Mukesh Haikerwal AC; General Medical Practitioner, Altona North.
Briefing submission: Mukesh Haikerwal
I would like to thank this chamber initiating this enquiry and grateful for the opportunity to speak to you today.
My name is Dr Mukesh Haikerwal and I am general medical practitioner in Altona North in Melbourne’s west. I’m just completing my 30th year in practice in this area.
In the appendix is a background of my career and advocacy.
I’m presenting this as a front-line general practitioner who has been involved in providing care the community locally across the State nationally and internationally.
The issues relating to Covid 19 need to be put into context regarding the whole response to this pandemic within our community and our state.
In our own practice we had to prepare for the GPs role in looking after people who potentially would be infected with Covid 19, how to exclude people from the clinic with respiratory disease so that this would not spread within our own workplace whilst providing care for them from testing, diagnosing, treating, providing supportive care, escalated hospital services, post hospital care.
The system initially was cumbersome.
After a test with a problem in our building that the doctor would then have to take the PPE of and sanitise. The room was then left closed and sprayed. It was then left closed for quite some time before we would consider it reasonable to reopen. The question of deep cleansing didn’t come in as the person did not test positive.
APPENDIX:
Dr Mukesh Haikerwal AC General Medical Practitioner T12, Circle Health Building, Unit 6, 230 Blackshaws Road Altona North, VIC 3025 Phone: +61 3 93933900 E: mckehaik@bigpond.net.au
Mukesh Haikerwal is a General Medical Practitioner in Altona North in the West of Melbourne, Victoria Australia. He is in a group teaching and training practice where he has worked since 1991 with his wife Karyn Alexander.
They worked with a partnership of 9 to build the “Integrated” North Altona Health Hub – Circle Health (www.circlehealth.com.au) and merged two local practices under the new Altona North Medical Group (www.anmg.com.au).
Part of their vision is CIRQIT Health (Community Innovation Research Quality and Information Technology – www.cirqithealth.com.au ) built on the upper floor.
The General practice includes a significant role in supporting patients needing psychiatric and mental health care in the area coordinating care with members of the Mental Health professionals’ network and beyond.
The 2020 COVID-19 Pandemic was a catalyst for change in Health and Health care delivery and as part of Mukesh’s highly public interventions including “Car-Park” testing, use of Video-consultations, deployment of lay “clinical Health Assistants” and “scribes” CIRQIT was the innovator, integrator and adoption agent for the “North Altona Respiratory Clinic”- a Federal initiative.
On 26 January 2018 he was made a Companion (AC) in the General Division of the Order of Australia for “eminent service to medical governance, administration, and technology, and to medicine, through leadership roles with a range of organisations, to education and the not-for-profit sector, and to the community of Western Melbourne.”
Of note, Mukesh has held high offices in Victoria, Nationally and internationally.
Mukesh is a passionate advocate for the use of technology in the health sector and stepped down as the National Clinical Lead and Head of the Clinical Leadership & Stakeholder Management Unit at Australia’s the National e-Health Transition Authority (NEHTA) after 6 years in August 2013. His roles there were in apprising the Australian community of the benefits of the vital role of IT in health care an enabler of progressive improvements and sustainability.
He worked for the Prime Minister of Australia on the National Health and Hospital Reform Commission formulating a future vision for Australia’s health including using eHealth as an enabler. He was previously assigned to the National Minister for Health’s eHealth Ministerial Advisory Group and had roles with the Victorian State government.
He was awarded the Order of Australia in 2011 for distinguished service to medical administration, to the promotion of public health through leadership roles with professional organisations, particularly the Australian Medical Association, to the reform of the Australian health system through the optimisation of information technology, and as a general practitioner.
He was the 19th Federal President of the Australian Medical Association, its Federal Vice President and, prior to that AMA Victorian State President. This saw him responsible for national policy development, lobbying with federal parliamentarians, co-ordinating activity across the AMA State entities and representing the AMA and its members nationally and internationally. He is a Life fellow of the RACGP and in May 2014, he was awarded the Gold Medal.
Canute was 40 when he died in 1035. He was also known as Cnut the Great, King of England, Denmark, Norway and parts of Sweden. By the time of the Norman Conquest in 1066 his story was quickly becoming lost to time but his relationship with the tide lingers on.about:blankEmbed URLPaste a link to the content you want to display on your site.EmbedLearn more about embeds(opens in a new tab)Sorry, this content could not be embedded.Try again Convert to link
Find following data as requested from the Royal Australian College of General practitioners.:
Practices (2019)
| NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust |
| 2 800 | 1 985 | 1 629 | 751 | 542 | 170 | 109 | 161 | 8 147 |
Source: Report on Government Services 2020 https://www.pc.gov.au/research/ongoing/report-on-government-services/2020/health
GPs (includes VR, non-VR, trainees) (2019)
| NSW | Vic | Qld | WA | SA | Tas | ACT | NT | Aust | |
| Headcount | 11,482 | 9,227 | 8,116 | 3,881 | 2,763 | 936 | 586 | 481 | 37,472 |
| FTE | 9,764.9 | 7,612.0 | 6,390.3 | 2,839.1 | 2,053.9 | 566.4 | 396.2 | 231.1 | 29,853.8 |
Source: Department of Health General Practice Workforce providing Primary Care services in Australia – Statistics by calendar year https://hwd.health.gov.au/CalendarYear.html
Community Health Centres: about:blankEmbed URLPaste a link to the content you want to display on your site.EmbedLearn more about embeds(opens in a new tab)Sorry, this content could not be embedded.Try again Convert to link
Victorian CHSs operate under two distinct legal and governance arrangements: 56 CHSs operate as part of public health services and 32 are independent registered CHCs.
The independent registered services are companies limited by guarantee, and registered under the Health Services Act 1988.
Primary Health Networks (PHNs).about:blankEmbed URLPaste a link to the content you want to display on your site.EmbedLearn more about embeds(opens in a new tab)Sorry, this content could not be embedded.Try again Convert to linkabout:blankEmbed URLPaste a link to the content you want to display on your site.EmbedLearn more about embeds(opens in a new tab)Sorry, this content could not be embedded.Try again Convert to link
6 Primary Health Networks in Victoria:
The Covidcare APPabout:blankEmbed URLPaste a link to the content you want to display on your site.EmbedLearn more about embeds(opens in a new tab)Sorry, this content could not be embedded.Try again Convert to linkabout:blankEmbed URLPaste a link to the content you want to display on your site.EmbedLearn more about embeds(opens in a new tab)Sorry, this content could not be embedded.Try again Convert to link
LEGISLATIVE COUNCIL LEGAL AND SOCIAL ISSUES COMMITTEE
Inquiry into the Victorian Government’s COVID-19 contact tracing system and testing regime
Transcript: Mukesh Haikerwal
Microsoft Word – FINAL-Contact Tracing 181120.docx (parliament.vic.gov.au)
Melbourne—Wednesday, 18 November 2020
(via videoconference)
MEMBERS
Ms Fiona Patten—Chair Ms Tania Maxwell
Dr Tien Kieu—Deputy Chair Mr Craig Ondarchie
Ms Jane Garrett Ms Kaushaliya Vaghela
Ms Wendy Lovell
PARTICIPATING MEMBERS
Dr Matthew Bach; Mr David Limbrick; Ms Melina Bath; Mr Edward O’Donohue;
Mr Rodney Barton; Mr Tim Quilty; Ms Georgie Crozier; Dr Samantha Ratnam;
Dr Catherine Cumming; Ms Harriet Shing; Mr Enver Erdogan; Mr Lee Tarlamis;
Mr Stuart Grimley; Ms Sheena Watt;
Necessary corrections to be notified to
executive officer of committee
Wednesday, 18 November 2020 Legislative Council Legal and Social Issues Committee 42
WITNESS
Dr Mukesh Haikerwal, General Practitioner.
The CHAIR: Hello, everyone. Welcome back. Today we are very pleased to be joined as part of the Inquiry into the Victorian Government’s COVID-19 Contact Tracing System and Testing Regime by Dr Mukesh Haikerwal, a GP in the west. Thank you so much for joining us today. Today with me I have Deputy Chair Tien Kieu, Ms Georgie Crozier, Dr Matthew Bach, Dr Catherine Cumming, Ms Kaushaliya Vaghela, Ms Wendy Lovell, Mr Enver Erdogan and Ms Melina Bath.
Just so you know today, Doctor, all evidence taken at this hearing is protected by law, and that is under our constitution as well as the Legislative Council’s standing orders. This means that it has parliamentary privilege.
However, if you were to repeat those comments outside you may not have the same protection. Any deliberately false evidence or misleading of the committee could be considered a contempt of Parliament.
Today we are recording and we have Hansard, who will provide you with a proof transcript. I would encourage you to have a look at that to make sure we have not misrepresented you in any way. Ultimately that transcript will be available on our website. We would really welcome you to make some opening remarks, and then we will have a broader committee discussion after that.
Dr HAIKERWAL: Thank you very much. I would like to thank you all for inviting me to attend the inquiry and to present and also for putting this inquiry onto the agenda. My name is Mukesh Haikerwal and I am a GP in Altona North. The end of the year is the end of my 30th year working as a GP in this area. I have taken the liberty of providing you with a written document with my details on the back of it, and I do not intend to read all of the pages before you. I would like to make some opening comments based on that, but really I would welcome any questions you might have of me.
I would like to start by saying that we are in a much better position now in Victoria than we have been. The height of our misery was in the middle of July, when we reached the 725 cases in a day, and we have reached 3500 health workforce participants who have been infected in this process as well. In my role as a general practitioner I have moved through various phases of this contagion, starting off with when we were not particularly aware of how significant it was going to become through to the first lockdown and then the second lockdown, and each of those parts of the journey have impacted directly in our practice, which is a large multidiscipline practice in the area, together with our respiratory clinic, which has been federally funded to provide the community with a testing service. It is not just a testing service but a service for people who have respiratory illnesses that otherwise could not be seen in the general practice to be seen and consulted with by a GP with full protective gear on so that they can then be looked after and treated without necessarily having to go to the emergency department. We also do testing and of course that is also a big part of this process.
One of the things we fundamentally brought here when we set up our clinic was the rigour of gathering the patient information and data to the extent that we deployed something called the national health identifier, which has to be very specific for the patient so we know we have got the right patient, right place, right time.
That has been instrumental in being able to see who is actually coming and where they are coming from, especially when they turn out to be positive, and that information has led us to the next stage: what happens when somebody turns up positive? We started testing on site on 3 April and we had zero cases until 2 July. On 2 July we had our first case and up until now we are at about 110 cases. There have been luckily no cases since the middle of October, I am really pleased to say. We have therefore interfaced with patients face to face prior to testing, during testing and after testing. We have written to every single one of their GPs electronically informing them of their results and about any outcomes of the consultations they will have had with us. We have had our services evaluated by the University of Melbourne—both the drive-through service, which is unique for Australia, and our respiratory clinic, which is one of over 140 across the country. We have made sure that we have given good service to the individuals by following them up, especially after they test positive, and that is how I know and feel the pain that they have gone through at each of the intervals that they have had.
We have had many constant problems throughout the process. I think we have worked through them with the department, and I think the most important thing for this committee that I can bring is what we had in what I would call our two local spikes in September to October. At that time we had on one site 22 cases that I reported in five days. I called the chief health officer after the first nine on day one and said, ‘Do you want me Wednesday, 18 November 2020 Legislative Council Legal and Social Issues Committee 43 to do something about this?’, and so we embarked on a process which I think is really useful, which is working with the local council, working with the local GPs and other providers in the area, and working with a very good branch of the health and human services department in the community testing and support scheme, which made us have a very direct impact on the local spikes. We tried to replicate these in other areas. I know that Wyndham is trying very hard in this area and I know I have reached out to other areas like Chadstone and Coolaroo when they had their outbreaks and indeed to my colleagues in Shepparton, and I think there is a lot to be learned from what has happened over here.
I am speaking to you as a frontline general practitioner. I have had a representative role for many years, and I continue to have, but really I am not speaking here with a political hat on but as a GP on the front line working with other GPs and other providers around here, all of whom are looking to improve the system and provide our support to the system to make sure the system works for us and for our patients so they get a decent set of support mechanisms when they are in this position of having contagion. We want to make sure they get their results when they need them, when they have had them, and make sure that there is a proper scheme so that in the future we learn from this and actually use all the people who are able to provide services, provide care, provide knowledge—local knowledge; intelligence, you might say—and make sure we have a system that we can be proud of.
I concluded on my little piece of paper—I am sorry, if there are any typos; I apologise. I have been putting in 16 hours a day since April around the clinics and so I have thrown this together, so if there are any mistakes, I beg your forgiveness right here, right now. We have a great system in evolution. We used to be the stand-out jurisdiction in the country doing health, and I want to make sure that we get back there. Thank you.
The CHAIR: Thank you, Mukesh. I think that is a goal that we all would like to achieve, and hopefully this inquiry assists us in making those recommendations to continue that improvement. I would also like to say I think, thanks to you, the systems are better now than they were. I think this is due to some of the things that you have highlighted this afternoon.
We had Professor Rait here on Monday, and his real concern was that lack of communication with general practitioners and with the patient’s own doctor. You were saying that when you do the testing at your clinic you ask the patient who their doctor is and you electronically send the results to them. Do you believe that that has been fixed? I mean, my understanding now is anyone who goes for a test is asked who their GP is and those results are sent through, but I am wondering if that is what you are hearing practically and on the ground.
Dr HAIKERWAL: No, I do not think it is fixed. I know there is a will to fix it. I know there is a direction to fix it. It does not mean it has been fixed. The pathology labs are very good at sending on copies to GPs if it is noted, but the systems that have underpinned some of the testing have not made that a matter of fact. I get reports from my local hospital, for instance, very well, but for patients who have been to other facilities to be tested, I do not tend to get their results in my general medical practice. I then have to go through that whole process of, ‘Where did you go? So who was testing it there? Which lab did they use at that site, not this site?
Which lab do I ring to try and get your results?’, and then I will try and get it electronically into my system. So no, I do not think it is there yet, but it certainly needs to get there.
The CHAIR: Yes. I certainly was at a testing site on the weekend, and they were asking those questions and putting it in—but not yet. That still seems to be one of our problems—well, a significant issue that could be improved. Where else do you think has been overlooked? I think certainly with Salesforce the government has been working but chasing its tail, it would appear, in this. Where else do you think that we really need to change—something that fundamentally improves our health system overall?
Dr HAIKERWAL: It is a fundamental problem with the relations between the federation. For some reason GPs are deemed to be the responsibility of the commonwealth and nothing to do with the healthcare system in Victoria or any other state. That is fundamentally wrong and flawed, because we are Victorians, we work with Victorians, we look after Victorians, we have 2 million people seeing a GP every day across the country, and we employ Victorians and we keep them healthy. So that is a fundamental problem.
I am afraid to state my age. I first started in 1991, where you are sitting now nearly, for something called the Brand report, which looked into healthcare—a report for Victoria. I was probably the only GP to turn up because nobody was bothered to go because they never report about general practice. I said to the Chair, ‘Why Wednesday, 18 November 2020 Legislative Council Legal and Social Issues Committee 44 haven’t you talked about general practice?’. They said, ‘It’s not part of our terms and it’s a commonwealth responsibility’. So it is fundamental. We have gone through many changes along the way where even the department has done some really good work about working with general practice, understanding the value that can be brought to the system with a joined-up system, making sure that people get the care where they need it and not necessarily having to be in hospital all the time. I think that this is something that is often spoken of but not operationalised, and in many of my years of advocacy this has been a key part of it, working with many good health ministers actually in the state and many good secretaries of health. I have literally walked and talked with them for years, and I do not think it gets beyond that level. That is the problem. It is in the fabric of the organisation, not necessarily in the higher echelons.
Toggle panel: eMember Protection options
No, Do not protect this content.
Yes, Protect this content.
Member
Associate Member
Affiliate
Covid and general practice is now live.
What’s next?Post address
By Mukesh Haikerwal
This is the “wash-up” of the COVID effort in our Respiratory clinic in Melbourne’s Western suburbs practice in Altona.
Below please find the link for the Report into the Contact tracing inquiry in Victoria. Your own exposure to this will be interesting in the New Year. None of us are out of the woods yet!
Below please find the link for the Report into the Contact tracing inquiry: your own exposure to this will be interesting in the New Year.
Read moreBy an AGPA writer
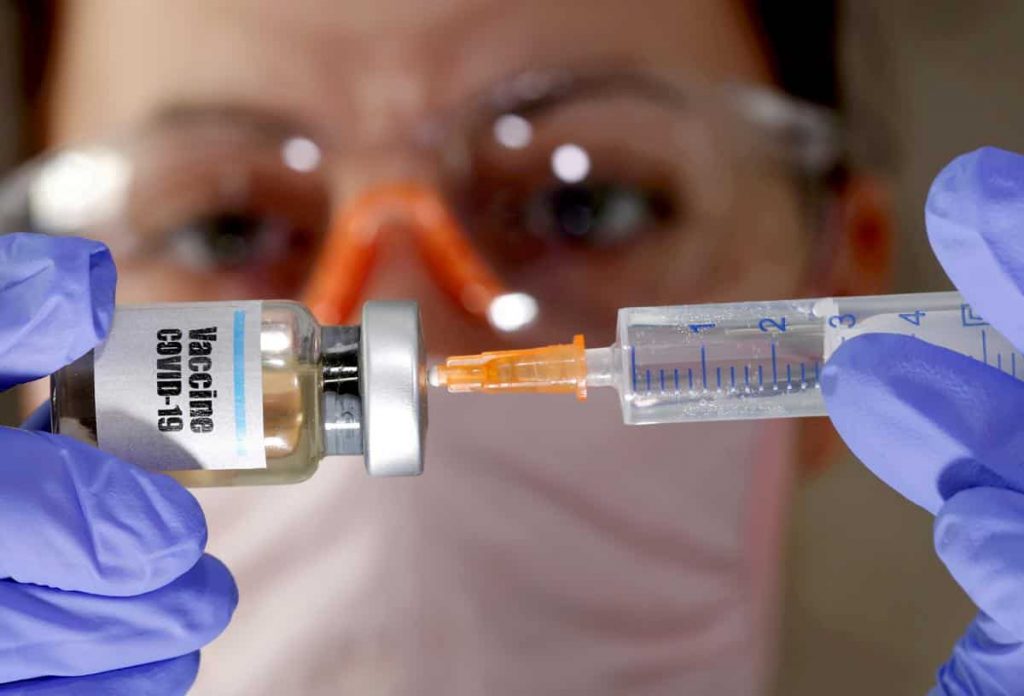
Pharmacists must be salivating at the thought of playing “a role in the wider Covid-19 vaccination roll-out from mid-2021”, in the words of a Department of Health official quoted by The Sydney Morning Herald.
Of course, the salivation is not over the modest fee for providing the vaccination. Rather it is because of the foot traffic into the pharmacy which these days sells everything from beach toys to mobile phone accessories.
Read moreBy Crispin Hull
In the past week the Federal Government renewed its commitment to extra funding for health care in rural and regional Australia and to extending training into smaller rural communities and rural residential aged-care facilities.
Answering a question in the Senate (2 December 2020) the Minister for Employment, Skills, Small and Family Business, Michaela Cash, stressed the need to move away from a one-size-fits-all approach.
This comes at a time when the Department of Health is working with the Royal College of General Practitioners and the Australian College of Rural and Remote Medicine so that the colleges take over the Australian General Practice Training scheme from the department.
Read moreGeneral practice businesses engaged with aged care will come under greater regulation if submissions by Counsel Assisting the Royal Commission into aged care are implemented.
Indeed, the regulation maybe prohibitive for some practices who might vacate the aged-care field.
Read moreAs the Federal Department moves towards handing the totality of the Australian GP Training Scheme to the colleges, the ultimate model for paying GP registrars remains in the air. At present, the registrars are employed by practice businesses on a base rate which is supplemented according to how many patients they see.
The GP Training Advisory Committee – a profession-led committee that advisory committee has put up for discussion a model in which the colleges employ the registrars.
Read more“It is with great sadness that we note the death of Dr Harry Nespolon”, Dr John Deery, Chair Australian GP Alliance, said today.
The Australian GP Alliance Board, on behalf of all members extends its deepest condolences to his partner and children, friends and colleagues.
“Harry lead the RACGP and represented the interests of General Practice with energy and commitment, and was particularly inspirational during the last six months where, despite a terminal diagnosis, he provided leadership for both the nation and the profession at a time of crisis”.
“General practice is the cornerstone of primary health care in Australia, and Dr Harry Nespolon understood the critical importance for General Practice to be both vibrant and viable to deliver the high quality of primary healthcare that Australians expect”, Dr Deery said.
“He worked hard to maintain funding at a critical time and to try to make sure that the small businesses that are GP Practices are viable business entities. Harry was well aware that unless these small business are viable the platform to deliver high quality primary healthcare will not exist, and the health of Australians will suffer accordingly.
“He also stood against attempts to reduce the quality of primary healthcare by opposing the use of paramedical personnel to diagnose and prescribe, despite determined lobbying from industry organisations representing the paramedical interests”, Dr Deery said.
General Practice has lost a committed leader, and while the profession will continue to deliver the healthcare that Australians need, for this moment we pause in reflection of a life well lived in support of Australia and the profession of General Practice.
Member Communication and Practice Support
As we mentioned in our December newsletter we have been working to try to improve communication and support our members who are spread across the country.
In February we trialled an online interactive seminar (read Webinar you can hold a discussion in) for the Queensland members and some other Queensland practice owners. The topic was Changes to the Cybersecurity Legislation and the Requirements for Reporting Security Breaches. We had a very good presentation from Redfish and a great discussion. Read more
Primary Health Care and Sonic Healthcare are an oligopoly present investment opportunity, according to an article by Graham Witcomb, an analyst with Intelligent Investor, in The Sydney Morning Herald. He writes that the growth in productivity of Australian pathology has been spectacular. Rebates for pathology have, in real terms, fallen by about 60 per cent since Medicare began in 1984, and yet the businesses delivering these services have done extremely well. Read more
The Australian General Practice Alliance was formed in 2016 to represent the interests of GP practice owners. While the initial trigger for the formation of the AGPA was the attacks on General Practice by the Australian Government and big business pathology, our aim is to address the issues that face principal led General Practices.
Read more »
You can download a PDF application for Full Membership here.
You can Join and Pay Online here »