GPs best for vaccination roll-out
By an AGPA writer
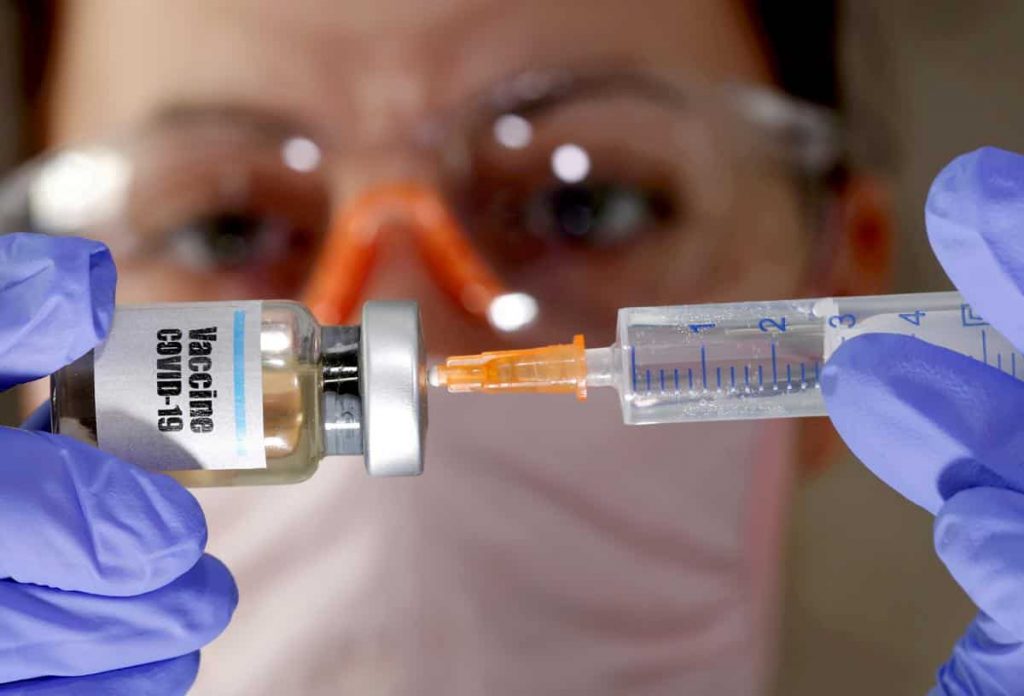
Pharmacists must be salivating at the thought of playing “a role in the wider Covid-19 vaccination roll-out from mid-2021”, in the words of a Department of Health official quoted by The Sydney Morning Herald.
Of course, the salivation is not over the modest fee for providing the vaccination. Rather it is because of the foot traffic into the pharmacy which these days sells everything from beach toys to mobile phone accessories.
The official might have overstated the official departmental stand. The official Australian Covid-19 Vaccination Policy says in the section on who, how and where the vaccinations will happen: “Pharmacists are licensed to varying degrees in each State and Territory to administer vaccines. They are likely to play a role in COVID-19 vaccination for some part of the population (e.g. healthy adults) at some stage, depending on the safety profile of the vaccines.”
The Australian COVID-19 Vaccination Policy (11 Dec 2020) is here.
Australian Medical Association President Dr Omar Khorshid said, “Pharmacy is an important part of primary care, but also a retail space trying to sell you products.”
The Government obviously wants as speedy a roll-out of the vaccine as possible. But any slow-down in getting to blanket vaccination will not come from long queues discouraging people to get vaccinated. Rather it will come from slow supply. It will be trickled out as the number of doses become available.
Indeed, this has often be the case with flu vaccines because flu vaccines have to be varied each season as the virus itself changes each season. Supply of flu vaccines invariably falls behind demand.
So as with flu, GPs, always at the front of healthcare, will easily be able to cope with the roll-out of the Covid vaccine.
Dr Khorshid said there were multiple reasons a COVID vaccination program should remain focused on GPs.
One concern was that the delivery of the COVID-19 vaccines was likely to be complex, with cold chain storage, multiple-dose vials and a requirement to enter all vaccinations on the national immunisation register.
He said general practice has the capacity itself to roll out a nation-wide program.
The policy, quite rightly places emphasis on delivery through general practice.
A further concern is that this is a new vaccine. Pharmacists will not be in a position to deal with adverse reactions. Even though the vaccine will have been thoroughly tested before the program begins, only mass-scale vaccinations will reveal all possible adverse reactions.
The policy recognises this and puts the emphasis on general practice in the roll-out.
The policy says: “Given that these are new vaccines, locations that have medical practitioners on-site are preferable for the first three to six months of the roll-out of any COVID-19 vaccine in case of adverse events.”
There would be a case for pharmacists to deliver the vaccine if without them blanket coverage would not be achieved as quickly. But it will be a case of supply not meeting demand for some time to come, rather than a case of vaccine supplies sitting on a shelf waiting for qualified people to administer them.
Further, patient visits to GPs for vaccinations usually have the worthy dual purpose of looking at patients’ overall health – something pharmacists are unqualified to do.
The only dual purpose the pharmacist supplies is to get an ancillary sale.
The well-heeled pharmaceutical industry – manufacturers, retailers and practitioners – has powerful lobby groups. It is therefore important that GPs remind policy-makers and MPs of the public-health importance of rolling-out the Covid vaccine via general practice and only to use pharmacies if they are absolutely necessary to get blanket coverage as quickly as possible.
For now, though, it looks like supply constraints mean that the roll-out could be done without any delay by using general practice (along with health workplaces and perhaps schools) as the first port of call.
Leave a Reply
Want to join the discussion?Feel free to contribute!